Overview – a hot, swollen, tender red leg could be a sign of cellulitis
Cellulitis is an acute spreading inflammation of the skin and subcutaneous tissues characterised by pain, warmth, swelling and erythema (inflammation).
When legs are swollen or there are other skin problems, the legs can sometimes become hot, inflamed and tender. Cellulitis typically only occurs in one leg.
It is very unusual for cellulitis to affect both legs at the same time so if there is redness or skin discolouration, pain and swelling in both legs, it is unlikely to be cellulitis. Cellulitis makes the skin painful, hot and swollen.
The area typically looks red or there will be a change in normal colour. It may be another condition commonly called Lower Leg Inflammation. For more information BLS Lower Limb Inflammatory Pathway (pdf download).
Symptoms – what are the symptoms of cellulitis?
The signs of cellulitis vary but things to look out for include:
- New redness or skin discolouration which may be spreading
- New or an increase in swelling
- Pain or tenderness
- Increased temperature in the area – the skin will feel ‘hot’ or like it’s burning
- Feeling generally unwell and ‘fluey’ is a common symptom, sometimes starting a few days before other symptoms
These symptoms can happen any time our lower legs and feet are swollen.
Sometimes infections are caused by damage to the skin such as a burn, cut, insect bite or even athlete’s foot. But often there isn’t always a visible trigger or cause of the infection. Cellulitis can be serious. If it is suspected the GP practice should be contacted promptly to get the correct diagnosis and start treatment as soon as possible.
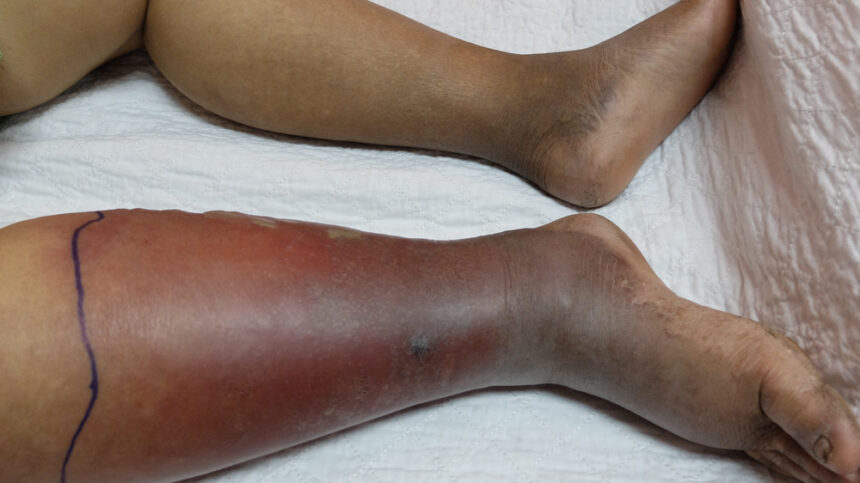
What does cellulitis look like?
Increased swelling, erythema, heat and pain in one leg.
Causes – what can cause cellulitis
A break/cut in the skin, fungal infections (eg athlete’s f00t), leg ulcer or insect bite can all cause cellulitis. But sometimes it can occur without any of these.
Swollen legs are more likely to get cellulitis because the lymph system is damaged or impaired and is not as good at preventing infection.
Diagnosis – getting diagnosed with cellulitis
If cellulitis is suspected it is important to get help straight away, especially if this is the first time with this problem. Ask for a same-day appointment with the GP. If the symptoms begin over a weekend, contact your out-of-hours GP service or NHS 111 or attend the local A&E.
The doctor or nurse will look at the affected area and make a note of the colour, swelling and temperature. They might also mark the area on the leg so it’s easier to see if your infection is getting better once treatment is started. They will also look for any wounds or other skin damage that might have caused the infection.
Most cellulitis infections are diagnosed by examining the leg or foot, but the doctor or nurse may also take a temperature or carry out some blood tests to confirm diagnosis. Cellulitis infections can look similar to blood clots (deep vein thrombosis or DVT) because of increased change in colour and swelling in one leg. Cellulitis can be confused with haemosiderin staining but this is redness or colour change without a temperature and should not be tender to the touch; another clue is that haemosiderin staining will not reduce or resolve with antibiotics. The doctor or nurse might refer on to the hospital to get further tests to make sure you get the correct diagnosis and treatment is accessed.
What to expect at the appointment
Cellulitis can be difficult to diagnose and to distinguish from other causes of inflammation in the legs but cellulitis most commonly affects one leg only. If there is a change in colour on both legs, it is likely to be associated with venous hypertension / insufficiency, swollen legs, and / or haemosiderin).
BLS Lower Limb Inflammatory Pathway (pdf download)
In lymphoedema / chronic oedema, attacks of cellulitis vary in presentation and may differ from classical cellulitis.
- Some episodes are accompanied by severe systemic upset, with high fever and rigors; others are milder, with minimal or no fever
- Increased swelling of the affected area may occur
- Inflammatory markers (CRP, ESR) may be raised
The initial assessment should include a baseline record to include the following:
- Extent and severity of rash – if possible, mark and date the edge of the erythema (this may be difficult in lymphoedema as the rash is often blotchy)
- Level of systemic upset
- Note history of repeated cellulitis, often a sign of unmanaged swelling
- CRP / ESR / white cell count – these may be helpful in diagnosis and monitoring of treatment
- Microbiology of any cuts or breaks in the skin – this should be considered before antibiotics are started.
Whether hospital admission is required will be decided by:
- The level of systemic upset and any signs of septicaemia
- Whether symptoms are worsening despite treatment
Treatment – what treatment will I be offered for cellulitis?
Antibiotic therapy
The length of antibiotic course for treating cellulitis in people with lymphoedema (swelling) in the affected leg may be longer than for standard management of cellulitis.
Symptoms may get worse in the first 48 hours of treatment, but should then start to improve. Call 111 if there is uncertainty or the GP is not available to ask advice on what to do next.
It is important that the whole course of antibiotics is finished. The length of antibiotic course for cellulitis, especially along with swollen legs, is often longer than antibiotic courses for other infections.
Sometimes a second antibiotic course or an extended course of antibiotics is needed just to make sure the infection has completely gone.
Managing pain
The infected area can be painful. Over the counter simple pain relief may be helpful along with rest and elevating the swollen leg or foot. Often people need time off work so a sick note from your GP might be needed.
Things you can do yourself
Whilst there is the acute infection you may need to rest, drink plenty of water and undertake your normal activity as able.
As well as taking antibiotics, you can help speed up your recovery by looking after your general well being. There are some approaches you can read on the NHS Choices’ website.
Remember that cellulitis is usually due to unmanaged swelling. If you normally wear a compression garment it might be too painful to wear during the infection. If it is, take it off – but you should try to start wearing it again as soon as you can tolerate it. You might need a different size stocking if the swelling has got worse during the infection.
But it is important to return to this important therapy as soon as you can. The team that provide your compression care and treatment will want to know about the infection so they can arrange a review appointment and make sure you are wearing the right compression garment.
Prevention – what can you do to prevent cellulitis and recurrent infections
Skin care
Your legs can become dry during and after the infection so make sure you keep them moisturised. Using an unperfumed moisturiser is better for your skin. There may be blisters or wounds that need dressing or monitoring by a nursing team so keep an eye out for those.
Reducing the risk of recurrence
The risk of further attacks of cellulitis in lymphoedema is high. Risk factors for recurrence of cellulitis in lymphoedema include:
- Swelling
- Cracks and / or maceration in between the toes
- Existing skin conditions eg dermatitis, eczema, psoriasis
- Open wounds including leg ulcers and fluid or even water filled blisters
- Inadequate compression therapy or not wearing your compression – if your compression is not comfortable, rolls, digs in, is too large, slips down, is too small, tight, causes pain, numbness, tingling, pins and needles, shortness of breath, marking on your skin or you cannot get it on or off with or without help, contact your Lymphoedema specialist or health care professional or GP
Make sure any existing skin conditions are treated as this will help to prevent recurrence. You may need to ask your GP for a referral to Dermatology.
Decongestive lymphatic therapy (DLT)
Lymphoedema intensive treatment (decongestive lymphatic therapy – DLT) is thought to reduce the frequency of attacks.
Preventative antibiotic therapy
If you have had an attack of cellulitis, you should carry a 2 week supply of antibiotics with you particularly when away from home for any length of time, eg on holiday. You should start antibiotics immediately if you observe familiar symptoms of cellulitis develop, but do seek a medical opinion as soon as possible. Inform your Lymphoedema Specialist and GP if you have a further episode of cellulitis.
If you have had two or more attacks of cellulitis per year your may be given antibiotics prophylactically. It may not be possible to fully prevent further episodes of cellulitis even with prophylactic antibiotics, however, there may be a reduction in the frequency of cellulitis and / or the severity of episodes.
Following one year of successful prophylaxis, it may be discontinued, particularly if the risk factors have been successfully addressed. However, if you have ongoing significant risk factors, continuing prophylaxis may be considered. Prophylaxis may need to be lifelong you have a relapse occurs after prophylactic antibiotics are discontinued.
Outlook for cellulitis
Cellulitis is a serious condition which can affect any part of the body but most commonly affects one leg.
If treated promptly with antibiotic therapy, you should make a full recovery and there should be no long term damage to your skin although some residual discolouration of the skin may persist.
Unfortunately, cellulitis cannot always be prevented and some people may have recurrent episodes. If this happens to you, it is imperative to undertake good skin care and avoid any breaks in the skin if at all possible.
Where’s the harm?
- Failure to treat cellulitis promptly may lead to septicaemia, which is life-threatening
- Failure to treat cellulitis adequately may lead to a cycle of apparently recurrent infections (when it is really a resurgence of the same infection) and increasing damage to the lymphatic system, causing unnecessary pain and suffering.
- Can lead to a waste of NHS resources, duplication of services, multiple appointments, inappropriate prescribed medications
- Overuse of antibiotics, prolonged courses with multiple changes, antibiotic stewardship and resistance. Side effects associated with antibiotics
- Each infection causes further damage to the lymphatic system and progression of oedema and associated skin and tissue changes
- Confusing cellulitis with lower limb inflammation or haemosiderin staining causes overuse of antibiotics and risks them being ineffective should they really be required in the future
Clinical guidelines for cellulitis
These guidelines give you a useful overview and more detailed information about cellulitis within the context of lymphoedema.
- BLS Lower Limb Inflammatory Pathway (PDF download)
- BLS Guidelines on the management of cellulitis in lymphoedema (PDF download)
- All Ireland Lymphoedema Guidelines 2022 (PDF download)
Cellulitis downloadable leaflet (PDF)
We’ve created a handy downloadable leaflet of the key information on this page so you can easily print it out for personal reference or to hand to a patient or healthcare professional. Or you can also simply forward it on by email.
Other support
The British Lymphology Society (BLS) is a dynamic and innovative body providing a strong professional voice and support for those involved in the care and treatment of people with lymphoedema and related lymphatic disorders, including lipoedema.
Contact details
01452 790178
admin@thebls.com
Find out more on the British Lymphology Society website
Lymphoedema Support Network (LSN) is a national UK charity which provides information and support to people with lymphoedema.
Contact details
020 7351 0990
admin@lsn.org.uk
Find out more on the Lymphoedema Support Network website
NHS Choices the official NHS website, which provides vital information and support about leg and foot signs and other symptoms.
Contact details
Call 111 - for non-emergency medical advice
Find out more on the NHS Choices website
Tell us what you think
If there’s anything you want to ask us or tell us, whether it’s a suggestion about our website, a complaint, or a compliment, drop us a line at
support@legsmatter.org










