Overview – dermatitis is a general term that describes a common skin irritation
Dermatitis can cause our lower legs to get inflamed or itchy. Dermatitis on the lower legs can often be caused by eczema. Eczema is a common skin condition that comes in many forms and affects people of all ages. It’s not contagious, so you can’t catch it from someone else.
There are various different types of dermatitis / eczema, so it’s good to be familiar with the different words used:
- Contact eczema / dermatitis – accounts for 70-90% or all occupational skin disease
- Atopic eczema – more common in children but you can also develop it for the first time as an adult
- Varicose or venous eczema – also known as ‘gravitational eczema’ or ‘stasis eczema’
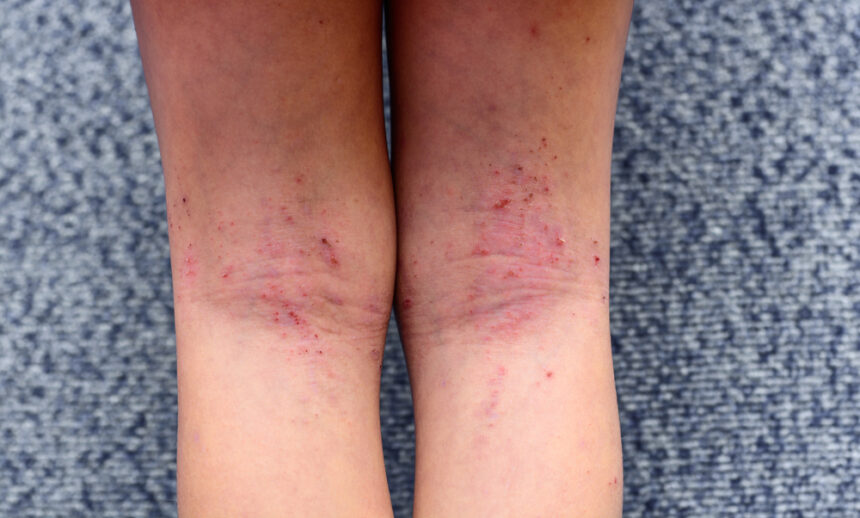
Eczema
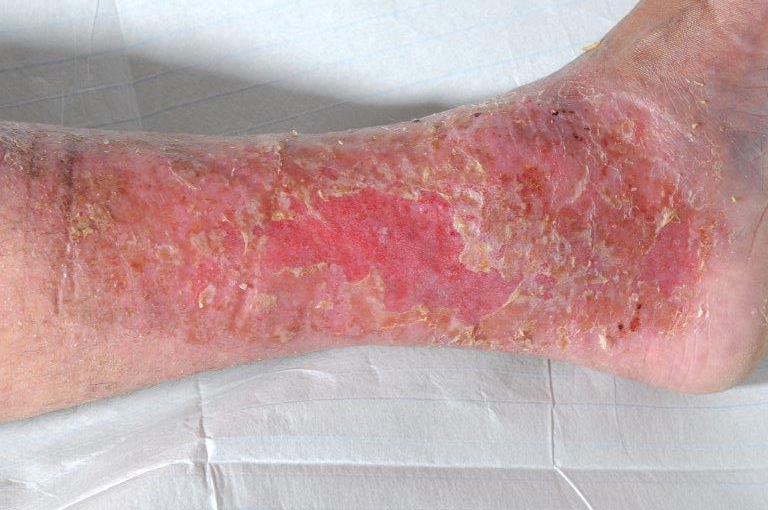
Varicose eczema
Symptoms – what are the key symptoms of eczema?
Varicose eczema is usually red and very itchy with scaly patches. Sometimes you may have patches that are also weeping or notice reddish brown staining above your ankle.
Further complications can occur from varicose eczema.
Cellulitis (skin infection) – There may be a spreading redness in the limb, swelling, pain, heat, pyrexia. The patient may be feeling unwell.
Contact dermatitis – It is possible that contact dermatitis can arise from reactions to treatments for venous eczema such as reactions to dressings or creams.
Causes – what causes dermatitis / dry, itchy skin?
Contact eczema / dermatitis
It is an iflammatory skin condition caused by external irritants such as body lotions and creams, or by clothing that contains wool. This can occur anywhere on the body.
Atopic eczema / dermatitis
It is not clear what causes atopic eczema but it often occurs in people who have allergies and can occur anywhere in the body.
Varicose eczema / dermatitis
Varicose eczema is a common cause of eczema on the lower leg which happens when high pressure in the veins in the legs pushes our blood into the skin tissue. This causes irritation. Not all dermatitis on legs is varicose eczema.
Diagnosis – getting diagnosed with varicose eczema / dermatitis
You can visit your local pharmacy in the first instance and speak to a pharmacist who may be able to assist, but you will need to contact your GP practice for an appointment.
You may be given an appointment to see the nurse rather than the doctor as nurses are often responsible for assessing patients with skin problems on the leg.
Alternatively, there might be a Leg Club or specialist leg clinic in your area. You don’t need to be referred by your GP to attend one of these.
Things to say when booking your appointment:
- Highlight if your skin is hot or red, this may be urgent and require care immediately
- Mention if your skin is cracked or there are pustules, blisters or weeping areas
- Say how the dermatitis started
- Make it clear if you have diabetes
- Make it clear if dermatitis has not healed within two weeks
- Let them know if there is an unpleasent smell or if your skin is painful and what makes this better or worse
What to expect at your appointment:
Medical history – your GP or practice nurse will try to determine the cause of the dermatitis/eczema by asking about underlying conditions such as:
- Diabetes
- Varicose veins
- Deep vein thrombosis (DVT)
- Injury or surgery in the affected leg
- Any eczema anywhere else on your body
- A history of skin problems
- Any new creams, washing powders etc
Examination – during your examination, the nurse or GP should:
- Ask about your symptoms and how long you have had problems
- Examine your lower legs to check for redness, swelling and / or signs of infection, pus, signs of heat
Tests – you may need some simple tests
- Doppler ultrasound – this test compares blood flow in your ankle with that in your arm to find out if there are blood flow problems in your lower leg. This is because problems with the veins in your legs can often cause varicose eczema. You might have to come back to have your Doppler test on another day or at another clinic but you should have this test within 2 weeks of your first appointment
- If you appear to have problems with your veins or arteries, you should be referred for further vascular tests which could include an ultrasound scan, CT scan or MRI scan to produce a detailed map of the blood circulation in your leg
- If your eczema is extensive, severe or difficult to manage, you will be referred to a Dermatology Clinic
- Other tests – this could include tests to check for other health problems that can affect your legs such as diabetes, lymphoedema, oedema, sepsis or cellulitis and anaemia
Treatment – what treatment will I be offered for dermatitis / varicose eczema?
If you have any form of eczema, the most important thing is to keep your skin clean and well moisturised. Avoid soap and washing with hot water as this can dry the skin and cause irritation, use warm water. Use a moisturising soap substitute when washing, bathing and showering.
After washing gently dry the skin, paying particular attention to the area between the toes. Avoid excessive rubbing to reduce friction and irritation. Ensure the skin is fully dry before applying a moisturiser (also known as an emollient). Applying the moisturiser in a downward motion, not against the hair growth, can help prevent irritation of the hair follicle. Allow the moisturiser to soak in for 20 minutes if possible before putting on clothes as this will help optimise absorption.
If you’re using moisturisers in the bath or shower, remember to also use a rubber mat or grip rail as the bathtub can become very slippery.
Sometimes, your skin may need more than just a moisturiser. Your doctor or nurse may recommend a steroid ointment or cream to be applied to the areas of eczema.
Steroid creams / ointments
These are powerful anti-inflammatories and are likely to be helpful. Potent steroid ointment can be applied to affected areas (daily or at dressing changes if a wound is present). Your Nurse or Doctor will advise you on what strength steroid is required, how often to apply, and how much to apply. Daily application is preferred in the first two weeks and then this is usually reduced gradually. When steroid creams or ointments are used underneath compression therapy, frequency of use is less; seek advice on amount and duration.
Compression therapy
If you have varicose eczema, it is important that the underlying cause is also treated and the most effective treatment is compression therapy.
Compression therapy improves the return of your venous blood supply by supporting the leg and foot. This can be done by wearing supportive socks or or tights or by bandinging the lower leg.
Compression therapy is very effective at reducing swelling, improving blood flow in the veins and healing or preventing varicose eczema. Compression therapy also reduces the inflammation in the skin thereby reducing pain and other skin changes you may see.
There are lots of different types of compression therapy so ask your nurse to find something that is right for you.
Compression can be a little uncomfortable when you first start treatment but should not cause you any pain. Any discomfort should reduce as the swelling goes down. If you do experience discomfort, talk to your nurse or doctor about it and they will advise you on ways of alleviating this.
If you are self-managing with hosiery or socks, then you should expect a treatment plan that includes what you need to do, how to recognise concerns and treatment check ins with the nurse.
Getting referred to a specialist
You may be referred if your GP or nurse is unsure about your diagnosis, or if you have eczema which is frequently troublesome.
Dermatology referral: If you have severe dermatitis or eczema which regularly causes problems, you should be referred to a Dermatology Specialist.
Tissue viability referral – a Tissue Viability Nurse is a specialist who considers all aspects of skin when complication in healing has occurred. In some areas they will be the first point of call for varicose eczema as they are also experts in compression therapy.
Vascular referral – if you have varicose eczema which is difficult to manage, surgical intervention from a vascular specialist might help your veins (the cause of the problem) and stop your eczema from coming back. Sometimes varicose veins can be treated by laser therapy. If you have peripheral arterial disease, you may require further investigations and the vascular team will be able to assess the need to improve the blood supply to your leg or whether your eczema can be managed in other ways such as reduce compression.
Questions to ask about your referral
- Is the doctor or nurse I will be seeing a dermatology, tissue viability or a vascular specialist?
- When will I be seen? Are you referring me as urgent or non-urgent?
- When will I have the tests?
- Who will give me the results and when?
- Who will help me manage my eczema while I wait for a specialist appointment?
Outlook – what’s the outlook for dermatitis / varicose eczema?
Varicose eczema is a lifelong condition where the underlying cause (high pressure in the veins) needs managing long term, usually with compression hosiery or socks.
There are simple procedures available on the NHS to treat the veins which are not working correctly, therefore, providing a permanent solution to your issues, avoiding the need to wear compression hosiery.
The need for good skin care is lifelong. Some people need to use topical steroids from time to time, but many people can prevent recurrent eczema with compression hosiery or socks and good skin care using emollients (moisturisers).
Prevention – how can you prevent eczema or dermatitis?
The main preventative measures for eczema or dermatitis are:
- Checking your legs regularly
- Following a comprehensive skin care routine
- Seeking advice early if you see anything unusual
- Eating a healthy diet and following advice about improving your mobility and/or exercising
Where’s the harm?
Inaction or insufficient action on varicose eczema or dermatitis can cause harm. This includes:
- Not checking legs and not doing basic checks, such as a Doppler test
- Not using adequate compression if indicated, can lead to worsening disease
- Not being referred to specialist services if required
Left untreated, varicose eczema can worsen and is at risk of becoming infected. If it is varicose eczema (not all dermatitis on legs is varicose eczema), you need to be offered the treatments above.
If you have any concerns about the treatment or care you are receiving, it is important to speak up.
Suggested resources for dry and itchy skin
These guidelines will give you a useful overview and more detailed information about venous eczema management:
- Gravitational eczema, varicose eczema (Web page)
- The NICE Clinical Knowledge Summary on venous eczema (Web page)
- A Patient Profession Reference article on venous eczema (Web page)
- Fact sheets from the National Eczema Society (Web page)
Dermatitis downloadable leaflet (PDF)
We’ve created a handy downloadable leaflet of the key information on this page so you can easily print it out for personal reference or to hand to a patient or healthcare professional. Or you can also simply forward it on by email.
Other support
The Lindsay Leg Club Foundation Promoting and supporting community based treatment, health promotion, education and ongoing care for people who are experiencing leg-related problems - including leg ulcers and other wound care issues.
Contact details
01473 749565
lynn.bullock@legclubfoundation.com
Find out more on the Lindsay Leg Club Foundation website
The National Eczema Society Formed in 1975, The National Eczema Society has two principal aims: first, to provide people with independent and practical advice about treating and managing eczema; secondly, to raise awareness of the needs of those with eczema with healthcare professionals, teachers and the government.
Contact details
0800 089 1122
helpline@eczema.org
Find out more on The National Eczema Society website
NHS Choices the official NHS website, which provides vital information and support about leg and foot signs and other symptoms.
Contact details
Call 111 - for non-emergency medical advice
Find out more on the NHS Choices website
Tell us what you think
If there’s anything you want to ask us or tell us, whether it’s a suggestion about our website, a complaint, or a compliment, drop us a line at
support@legsmatter.org










