Overview – lymphoedema is a long-term (chronic) condition that causes swelling in the legs and / or feet
Sometimes our legs or feet become swollen and feel uncomfortable. This is known as oedema and it happens when fluid in our lower legs or feet has trouble returning back up through the body. It may be a temporary problem such as after a long flight when it is a way of our body telling us we need to move around more. It is the lymphatic system of vessels, like veins, that work to remove this excess fluid and along with it, various toxins that the body needs to excrete via the kidneys.
However, for the lymphatic system to do its job well, needs to be stimulated by regular movement of muscle and skin. Temporary swelling is a sign that we need to move around a bit more and stretch our ankles and calf muscles. It usually goes away quite quickly once we start to move around.
If swelling of the feet, ankles or legs persists for more than 3 months it is called chronic oedemaAlthough there are several causes of chronic oedema which need to be treated, oedema that does not completely resolve overnight or with elevation, indicates that the function of the lymphatic system is beginning to fail and is a sign of early lymphoedema (lymphatic failure).
All chronic oedema, regardless of initial cause, indicates a degree of lymphoedema. If not treated, it can lead to changes in the skin and deeper tissues. It can also lead to infection (cellulitis). Lymphoedema in the lower limbs is commonly related to chronic venous insufficiency.
Symptoms – swollen legs and feet
What does oedema look like?
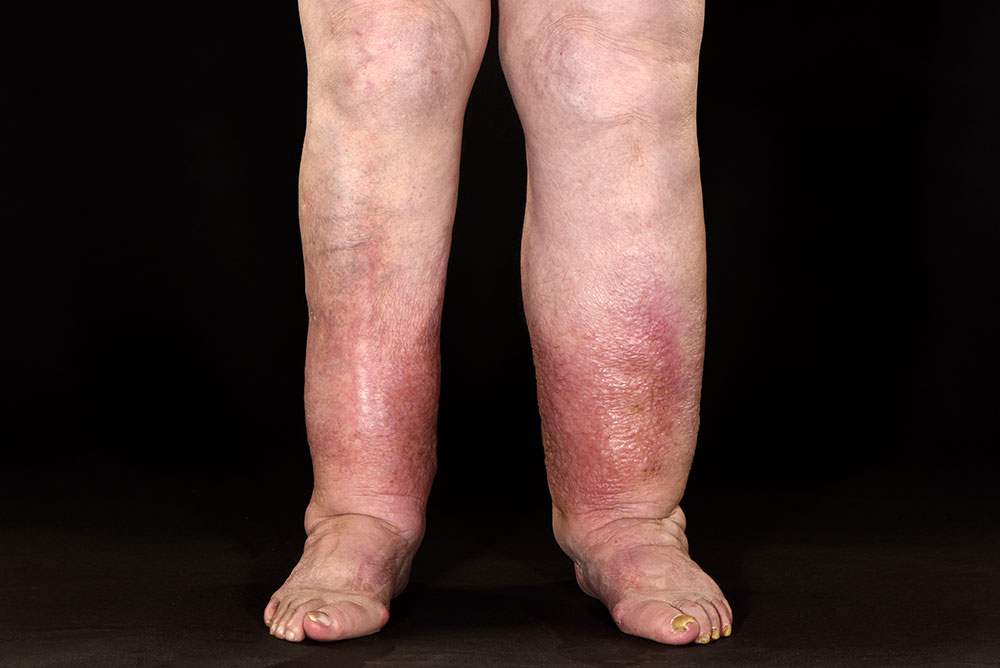
The first sign of oedema is swelling which can occur in one particular part of the body (for example the feet or ankles), or may be more general, depending on the cause. It can also cause feelings of tightness, discomfort and stretching of the skin.
The above image shows chronic oedema of the legs and feet. We know it is chronic and that there is lymphatic failure because of the deep skin folds which have developed due to the tissues under the skin become thickened and firmer in an uneven way. There are also skin changes with a blistered or warty appearance, but the skin may also look dry and scaly. The risk of developing an infection called cellulitis is also increased.
Causes – what can cause legs and feet to swell?
Lymphoedema
The lymphatic system can be thought of as a waste disposal system that takes tissue fluid and waste products away from the tissues around your skin, fat, muscle and bone.
Once the tissue fluid is inside the lymphatic vessels, which are just under the surface of our skin, it becomes known as ‘lymph’. Lymph is then transported in one direction by larger and deeper lymphatic vessels.
Lymph moves when we are active and when we breathe deeply, so any physical activity helps the lymph vessels work better and prevent or reduce any swelling. Being active is an essential part of treatment.
Some people may be born with a tendency to develop it because of the way their lymphatic system formed. However, it may arise for many other reasons which cause the lymphatic system to find it difficult to work properly such as problems with our veins, repeated infections (cellulitis), cancer treatment involving surgery or radiotherapy in the pelvis or lower limbs.
Some joint surgery may also damage lymphatic vessels and contribute to development of lymphoedema. However, the biggest risk factors for developing lymphoedema are being overweight and inactive so it is vital to address these issues as part of the management of the condition.
Any form of swelling which does not reduce and has been present for longer than 3 months suggests there is a problem with the lymphatic system and could be called lymphoedema. There are therefore many causes of lymphoedema so it is important that a good assessment is carried out to make sure the best treatment is being given depending on the cause of the problem.
Here’s a short film to explain “What is Lymphoedema?”.
Venous hypertension
‘Venous’ is anything related to our veins. Swelling often happens when our veins are not working as well as they should. Blood is pumped from our heart to the rest of our body through our arteries and returns to our heart through your veins. Blood is then propelled back to our heart by our heart pumping. Our leg and foot muscles help this along by circulating blood as you walk and move your ankles.
Our veins contain one-way valves that stop the blood falling back towards your toes. These valves can become weak or damaged. When this happens, our veins become swollen (varicose veins) that blood is forced into the tissue of our skin making it swell and overburdening the lymphatic system.
Cardiac oedema
Swelling in the lower legs can also be caused by right-sided congestive heart failure. This is known as cardiac oedema and also causes shortness of breath and weight gain. It is important that cardiac oedema is considered in anyone being treated for these symptoms, and before compression therapy is prescribed.
However, if someone has a cardiac problem they may also have other problems, such as lymphoedema which must be treated too. If treatment for a cardiac problem does not resolve chronic foot or ankle swelling, this is a strong indication that the lymphatic system has not been able to cope with the chronic overload of fluid and lymphoedema has developed.
You can read more about lymphoedema at NHS Choices, on the British Lymphology Society pages or on the information pages of the Lymphoedema Support Network.
Diagnosis – getting your lymphoedema diagnosed
If your legs or feet are swollen, it is necessary to make an appointment with the GP practice, who will be able to diagnose or exclude conditions such as cardiac problems. The GP may make a referral to a nurse responsible for caring for patients with venous leg problems or a lymphoedema clinic.
The nurse or doctor should:
- Assess the legs – if there are signs of cellulitis, an urgent medical referral is required. Please also refer to the BLS / LSN guidelines on the management of cellulitis in lymphoedema (PDF)
- Assess possible risk factors for venous insufficiency, arterial disease, lymphoedema
- Exclude lipoedema as a possible diagnosis
- Perform a clinical assessment for significant arterial impairment. This may include, but should not be solely based on, measurement of Ankle Brachial Pressure Index (ABPI), particularly because a reading may not be possible in a swollen limb
- If there is leakage of lymph from the legs, this needs treating promptly to stop the problem getting worse by breaking down the skin further or increasing the risk of celllulitis. Please refer to the The chronic oedema wet leg pathway (PDF) Advice on skincare is also required, together with appropriate dressings to absorb the leakage and some form of appropriate compression to help stop the leakage
- If problems with the veins or arteries are suspected, a referral should be made for further vascular tests to check if (modified) compression therapy and/or intervention to the veins or arteries is appropriate
Other tests may be required to check for additional health problems such as diabetes and anaemia that can affect the legs or to exclude any problems in the pelvis which could be preventing the lymphatic system from effectively working.
The GP Practice may make a referral to a specialist lymphoedema clinic or to a local hospital if they suspect problems with the veins or arteries.
If signs of infection (cellulitis) occur, eg redness, more swelling, pain, and feeling fluish, seek medical advice immediately.
Treatment – what treatment will I be offered for lymphoedema of the legs?
The treatment for swollen legs depends on what has caused the swelling. The earlier the cause of oedema is identified and treated, the better the outcome. With prompt, appropriate treatment, swelling will be reduced, wounds will heal more quickly and complications, such as cellulitis, will be avoided.
Compression
If the legs or feet are swollen because of venous insufficiency or lymphoedema and there are no problems with the blood supply to the legs or feet, then compression therapy is a key part of treatment.
Compression therapy improves blood supply by applying pressure to the leg. This can be done by bandaging the lower leg or by wearing supportive socks, stockings or tights. Compression therapy is very effective at reducing swelling, reducing the risk of cellulitis and healing or preventing sores or ulcers. Referral to a lymphoedema or other specialist for specialist measuring and fitting of compression may be needed.
There are lots of different types of compression therapy so it is important to discuss the different types and specific needs to make sure the best option is prescribed. Legs may feel uncomfortable at times in compression stockings or bandages. This is often towards the end of the day when the legs can become more swollen. This can be relieved by elevating the legs for a good amount of time and stretching the ankles and calf muscles and wiggling toes can also help.
If pain relief has been required, eg for an ulcer, it is best to continue with this until accustomed to the compression treatment. Compression stockings or bandages should not increase pain. If pain increases or becomes severe, it should be reported to the nurse or doctor who prescribed them.
Compression bandaging should be applied with caution if there are signs of:
- Severe arterial disease
- Untreated deep vein thrombosis (DVT)
- Uncontrolled heart failure
- Uncontrolled hypertension
- Severe peripheral neuropathy
- Cellulitis – compression may be suspended or reduced for a few days if normal compression cannot be tolerated but should be restarted as soon as possible to stop any further swelling developing
Compression garments
Compression garments are usually the mainstay of long term treatment. Generally, higher levels of compression are needed when treating lymphoedema than if treating venous oedema alone (minimum RAL Class 1 (18-23mm Hg).
Flat knit and / or custom made garments are often used. This is because lymphoedema changes the shape of the limb so off-the-shelf garments can create a tourniquet effect, which exacerbates swelling. It it is important that garments fit well and are the correct ones for the individual. There are lots of options available so discussing these and the individual patient needs are essential.
Multi-layer lymphoedema compression bandaging (MLB)
Bandaging is an alternative to compression garments. Short-stretch bandaging is generally used to create a low resting pressure and high working pressure. Bandaging is appropriate if:
- Skin is fragile, damaged or ulcerated or there is lymphorrhoea (weeping skin)
- There are chronic skin changes, e.g. hyperkeratosis or papillomatosis
- There is distortion in shape or exaggerated skin folds
- The affected limb is too large to fit hosiery
Compression wraps
Wraps may also be recommended alongside other treatment or as an alternative to compression garments or bandaging (as long as there is minimal or well-managed leakage). Sometimes if it is physically difficult to apply stockings, or long term bandaging is not an option, then a wrap might be very helpful.
Lymphatic drainage
This is a specialised light massage technique that stimulates and reroutes lymph flow to viable drainage areas. A lymphoedema specialist will be able to decide if an individual may benefit from either a course of Manual Lymphatic Drainage (MLD) or learning how to undertake a modified version of this, which is called Self Lymphatic Drainage (SLD)
Other adjunctive therapies that may be considered include sequential pneumatic compression, kinesiotaping or low level laser therapy. These all need to be carried out by practitioners with specialist training.
Things you can do to help prevent and manage lymphoedema
Although lymphoedema or chronic oedema can not necessarily be prevented we can definitely reduce the risk of it developing it. Seek advice if there is any swelling in your legs – prompt action always helps and it may be the reason for the swelling being treatable.
Here are some lifestyle changes you can make to help reduce swelling:
- Learn how to care for your skin and prevent cellulitis. Swollen tissues are easily damaged, so care is needed to protect skin from injury, scratches, insect bites or sunburn. Lymphatic failure increases risk of infection, so keep skin clean by washing and careful drying, especially between the toes daily and applying a non-perfumed moisturiser to keep the skin supple
- Adopt and maintain a healthy diet and weight
- Be as active as possible. The ideal is to take light to moderate exercise such as swimming or walking for about thirty minutes at least three times a week. Being active while wearing compression is particularly effective. Even if with limited mobility, there are things that can be done to help to reduce swelling. Refer to the British Lymphology Society EveryBodyCan pages for ideas and information
View Legs Matter Movement videos - Avoid standing for a long time – it is best to keep feet and legs moving as much as possible. A good activity is to try lifting up one heel at a time to stretch the foot arch or rock back on the heels but make sure there is something to hold on to avoid any falls
- Avoid sitting for long periods with legs down, put feet up – elevating legs above the level of the heart. It is also helpful to do foot and ankle stretches to help the circulation of blood and lymph
What’s the outlook if you have lymphoedema
The earlier the cause of oedema is identified and treated, the better the outcome. With prompt, appropriate treatment, swelling will be reduced, wounds will heal more quickly and complications, such as cellulitis, will be avoided.
Harm – the risk factors
Inaction or insufficient action on oedema and lymphoedema can cause harm. This includes:
- Swollen ankles and feet may seem like a trivial problem that affects us all as we get older. However, it is a warning sign that something isn’t working properly, eg the heart, kidneys or possibly alongside a failure of the lymphatic drainage system
- Ignoring the symptom allows the damage to get worse and be harder to treat in the longer term
- Lymphatic drainage failure (lymphoedema) that is untreated causes changes in the skin and the tissues under the skin and puts the person at risk of a serious infection called cellulitis, possibly leading to septicaemia.
If you have any concerns about the treatment or care you are receiving, it is important to speak up. Find out more.
Resources
- What information, advice and support should be provided for those at risk of lymphoedema? (Web page with option to download PDF for members)
- Lymphoedema facts, activity and exercise (Web page with option to download PDF)
- Get moving with lymphoedema (PDF Download)
- An ‘easy read’ document all about lymphoedema for people with learning difficulties (PDF download)
Oedema and lymphoedema downloadable leaflet (PDF)
We’ve created a handy downloadable leaflet of the key information on this page so you can easily print it out for personal reference or to hand to a patient or healthcare professional. Or you can also simply forward it on by email.
Other support
Some organisations you can contact for further information.
Accelerate Based in East London, Accelerate can accept national referrals from your GP / specialist to our world-class centre where we pioneer and trial experimental new treatments for chronic leg ulcers / wounds, lymphoedema and mobility challenges.
Contact details
020 3819 6022
hello@acceleratecic.com
Find out more on the Accelerate website
The British Lymphology Society (BLS) is a dynamic and innovative body providing a strong professional voice and support for those involved in the care and treatment of people with lymphoedema and related lymphatic disorders, including lipoedema.
Contact details
01452 790178
admin@thebls.com
Find out more on the British Lymphology Society website
Lymphoedema Support Network (LSN) is a national UK charity which provides information and support to people with lymphoedema.
Contact details
020 7351 0990
admin@lsn.org.uk
Find out more on the Lymphoedema Support Network website
NHS Choices the official NHS website, which provides vital information and support about leg and foot signs and other symptoms.
Contact details
Call 111 - for non-emergency medical advice
Find out more on the NHS Choices website
Tell us what you think
If there’s anything you want to ask us or tell us, whether it’s a suggestion about our website, a complaint, or a compliment, drop us a line at
support@legsmatter.org