Overview – what are sickle cell leg ulcers?
Leg ulcers can occur in people already diagnosed with sickle cell disease. These can be nasty ulcers and add to the pain and debilitation that having sickle cell disease brings.
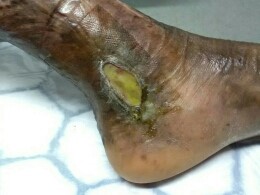
Symptoms – what are the symptoms of sickle cell related leg ulcers?
Sickle cell ulcers usually show around and behind the ankle, they can also present around the base of the toes in more extreme cases. They can be single ulcers or multiple and can occur in both legs at once. The ulceration is usually painful and adds to the general debilitation for people with sickle cell disease.
Sickle cell ulcers often deteriorate during a sickle crisis due to the general reduction in oxygen to the skin. Tolerance of treatment may be difficult. Neuropathic pain and hypersensitivity around the ulcer may also be extreme.
Causes – what causes sickle cell related leg ulcers?
The cause is complex but is thought to be related to the sickled red cells causing obstruction to the small blood vessels, reducing oxygen to the skin and venous incompetence. Pain within sickle crisis can also reduce mobility and may cause stiffening of the ankle, thereby reducing venous function further. The combination of all these factors can create the environment for an ulcer to develop followed by infection and inflammation.
Why can sickle cell disease cause leg ulcers?
Sickle cell related ulcers may be more common in men or those with chronic anaemia due to a severe rate of haemolysis. This condition may present in teenage years but more commonly in their 20’s to 30’s. This can create a major disruption to their employment.
Diagnosis – how to diagnose sickle cell related leg ulcers
Leg ulceration can occur more often in individuals with lower haemoglobin. The ulcers usually present around the medial and lateral malleolus (your ankle). Ulcers are also common to the toes and dorsum of the foot.
If you knock or experience trauma and a wound to your leg, ask your GP to refer to your local leg ulcer team for a full lower limb assessment as well as a vascular referral. It is important to commence compression therapy as soon as you experience a wound to your lower limb.
You may experience high pain from the ulcer and therefore also discuss with your GP pain relief while you are waiting to be assessed.
Your GP, Leg Ulcer Clinic and Haematology department will need to work as part of a Multi-Disciplinary Team (MDT) to manage your SCD and ongoing wound management (for example pain, wound care and medical management).
Treatment – how to treat and manage sickle cell leg ulcers
Treatment can be trickier simply because you will also have the other side effects of sickle cell disease that you are trying to manage. It’s likely you will also have a concoction of general medication and you may also be trying to minimise the impact of this ulceration on your employment.
Please talk to your healthcare professional about these complexities so that they can be taken account of within the management plan.
Treatment requires the following important interventions:
Medical management of sickle cell leg ulcers
Medical management with a haematologist to ensure your sickle cell disease is managed as well as it can be.
Pain management for sickle cell leg ulcers
You may need medication for nerve related pain (neuropathic pain); this can result in a sharp or burning pain and may not be managed with standard pain killers. Make sure you describe your pain to your doctor.
Compression therapy of sickle cell leg ulcers
Compression therapy may be bandages, socks or wraps. Compression is an essential part of the treatment if you have ulcers on your legs or feet and can get forgotten. Medical management may not be enough on its own to control this condition. Even if your leg is not very swollen the compression bandage or sock will reduce the level of fluid leaking from the ulcer(s).
You may want to start with mild compression, but if you have a large wet ulcer, try to ensure you get a stronger level of compression. This will also work to reduce the local inflammation and is critical part of the treatment for this condition. In severe cases of lower leg ulceration, elevation and even bed rest initially may be essential.
Review of your walking and footwear
Seek a review of your walking and footwear if you believe this is becoming a problem. During crises your mobility will reduce and your ankle may stiffen. It is essential to keep stretching your ankles and that you try not to ‘walk on your toes’. There is a high risk of foot and ankle deformity associated with sickle cell ulceration; this must be addressed early to prevent this. You may need special exercises and orthotics for your shoe.
What can reduce healing of sickle cell and leg ulcers?
The site of the ulcer can make the standard compression therapy less effective. If your ulcer is behind the ankle, the compression bandage or sock will not generally apply the level or dosage of compression to the wound bed that it requires to heal. If your ulcer is failing to heal with compression, seek help from your local Tissue Viability Nurse. Ask about the application of special padding to the ulcer behind the ankle or the use of compression strapping.
If you’re quite tall and you have a long leg, then you may also need extra strong compression to heal. Again, seek help from your local Tissue Viability Nurse.
Outlook for sickle cell leg ulcers
Sickle cell ulcers can deteriorate during a sickle crisis so need careful management between healthcare providers. Ulcers can be extremely painful therefore making therapeutic compression difficult.
With the correct treatment, ulcers can heal but after healing will need continued management with compression hosiery (socks or wraps) to reduce recurrence and may require higher compression if tall or a longer limb.
Prevention of sickle cell leg ulcers
If you have sickle cell disease, make sure you look after your legs and avoid lower limb trauma where possible.
Seek medical attention as soon as you notice a break in your skin to the lower limb – so treatment can commence and prevent further breakdown.
Elevate legs regularly to prevent venous complications and where possible wear compression hosiery as a prevention.
Harm – the risk factors
Sickle cell ulceration on the legs needs compression therapy alongside the medical management. The powerful anti-inflammatory effects of compression therapy can get missed whilst the doctors focus on establishing the correct medication and pain relief. While sickle cell ulcers are not caused by venous hypertension, it is clear that the ankle mobility is reduced thus impacting on venous return; any wound on the leg heals faster with compression therapy.
Resources
The Sickle Cell Society (Website)
Sick Cell Anaemia News (Website)
Sickle cell leg ulcers downloadable leaflet (PDF)
We’ve created a handy downloadable leaflet of the key information on this page so you can easily print it out for personal reference or to hand to a patient or healthcare professional. Or you can also simply forward it on by email.
Other support
Some organisations you can contact for further information.
Accelerate Based in East London, Accelerate can accept national referrals from your GP / specialist to our world-class centre where we pioneer and trial experimental new treatments for chronic leg ulcers / wounds, lymphoedema and mobility challenges.
Contact details
020 3819 6022
hello@acceleratecic.com
Find out more on the Accelerate website
Mind Mind is the UK’s leading mental health charity. They're there to make sure no one has to face a mental health problem alone you can call or text for free anytime.
Contact details
0300 123 3393 or text 86463
info@mind.org.uk
Find out more on the Mind's website
NHS Choices the official NHS website, which provides vital information and support about leg and foot signs and other symptoms.
Contact details
Call 111 - for non-emergency medical advice
Find out more on the NHS Choices website
Samaritans Samaritans are there 24 hours a day, 365 days a year providing emotional support to anyone in emotional distress. Call them free any time, from any phone.
Contact details
116 123
jo@samaritans.org
Find out more on the Samaritans' website
Tell us what you think
If there’s anything you want to ask us or tell us, whether it’s a suggestion about our website, a complaint, or a compliment, drop us a line at
support@legsmatter.org










