Pyoderma Gangrenosum (PG) is a rare but treatable skin or dermatological condition that can cause leg ulceration and and needs to be diagnosed by a Dermatologist. A diagnosis of Pyoderma Gangrenosum can be quite scary but like all conditions, having a diagnosis is the first step to getting the correct treatment so that the wound heals.
It can happen anywhere on the body – it can start spontaneously or even start following a surgical procedure. Pyoderma Gangrenosum lesions or wounds on the leg are often slow to heal simply because wounds on the legs heal more slowly that other parts of the body, especially if there is any lower leg swelling. PG can be very painful and can deteriorate fast thus getting the correct diagnosis and treatment plan is critical.
Medical management includes a range of anti-inflammatory medication plus pain relief. However, if the ulceration is on the leg it is very important to have some form of compression bandaging to support the leg and reduce swelling and wound exudate.
Despite its name, it is not a type of gangrene. Pyoderma Gangrenosum is not contagious and cannot be passed from person to person.
Symptoms – what is Pyoderma Gangrenosum?
The condition usually starts with one single ulcer; this can unfortunately deteriorate quite quickly to a large or deep wound. Occasionally there may be multiple ulcers. Pain or discomfort from the ulcer is common from the outset.
How the ulceration presents is dependent on your skin tone. For those with lighter skin tones, the edge of the ulcer initially may look purplish, for those with darker skin tones the ulceration may look darker. Sometimes the person may remember that it started like a raised or red nodule or blood blister – sometimes people think they had a nasty insect bite. Pyoderma Gangrenosum is not a skin cancer and does not lead to cancer.
What does Pyoderma Gangrenosum look like?
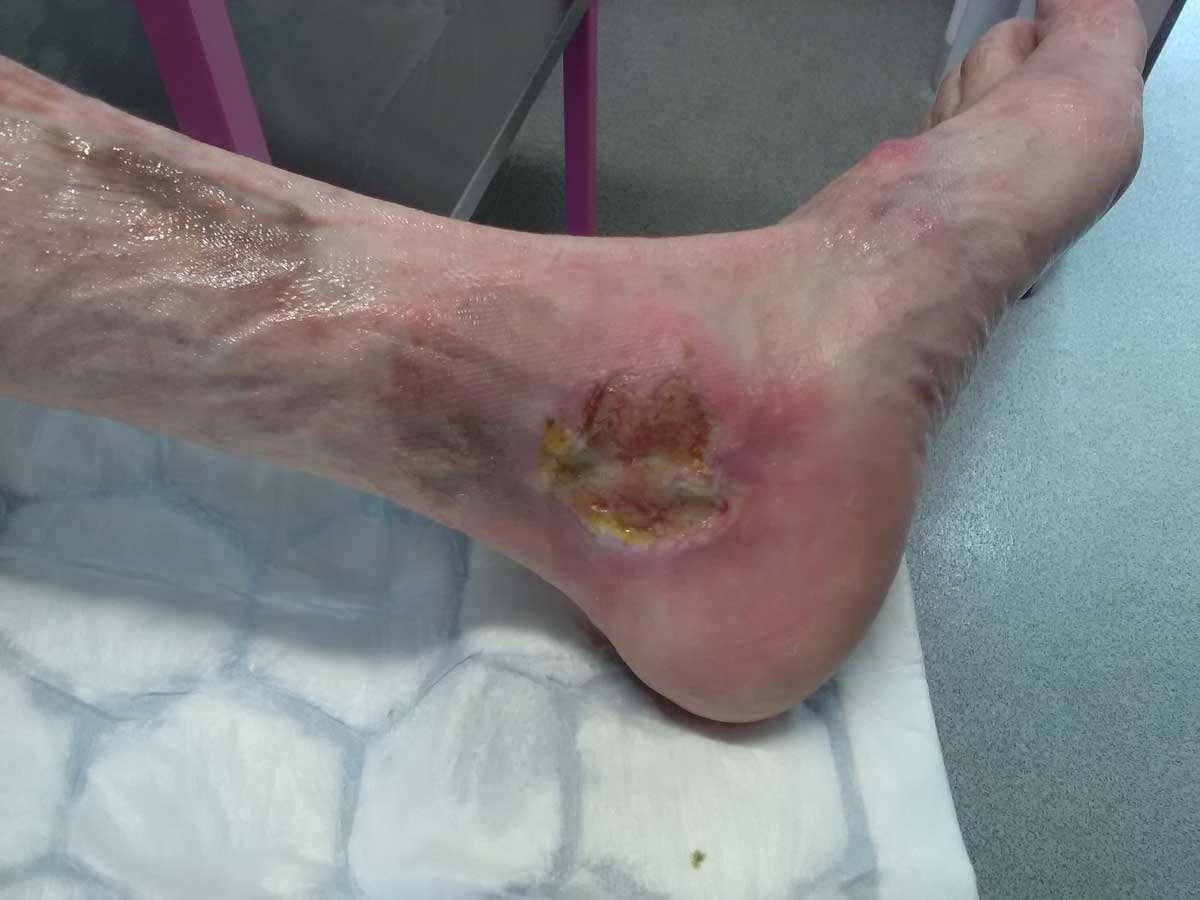
Causes – what can cause Pyoderma Gangrenosum?
The cause of Pyoderma Gangrenosum is often unknown. Approximately half the people diagnosed have no known cause for it. It may start after trauma to the skin. Pyoderma Gangrenosum can sometimes be associated with an underlying medical condition such as inflammatory bowel disease, arthritis or certain blood disorders. It is important to know that having Pyoderma Gangrenosum does not mean that you have these conditions but your specialist or doctor will consider and exclude these.
Diagnosis – getting diagnosed with Pyoderma Gangrenosum
There is no specific blood test for Pyoderma Gangrenosum.
If your nurse or doctor thinks you might have it, they may ask for some tests, including:
- Taking a small sample at the edge of your wound (biopsy) to establish the presence of Pyoderma Gangrenosum or help rule out other causes of skin ulcers
- Taking a swab of the wound to check for any infection
- Blood tests to check for conditions associated with Pyoderma Gangrenosum
If Pyoderma is suspected you should be referred onto a specialist, usually a dermatologist who will confirm a diagnosis and advise you on treatment options.
Pyoderma Gangrenosum can be difficult to diagnose because it does not always show the classic signs of the disease, it may be confused with other conditions and even the biopsy may not detect it.
Providing a diagnosis of Pyoderma Gangrenosum can be tricky. It is often described as a ‘diagnosis of exclusion’ in other words, other diagnoses have been excluded and the diagnosis of PG is suspected. If the lesion responds to medication, then it is presumed to be caused by Pyoderma Gangrenosum.
Thus it becomes important to try and describe your pain to the medical and nursing team, especially if servere.
Treatment – how to treat Pyoderma Gangrenosum
Pyoderma Gangrenosum is often difficult to treat and may take some time to heal, especially if the lesions are on the lower leg. Treatment requires the following important interventions.
Medical management by a Dermatologist
The consultant aims to get the inflammatory condition under control. Oral medication may include steroids, special antibiotics OR immunosuppressive medication. A topical steroid ointment may be applied directly to the wound. More than one treatment may need to be tried; this will be based on the patient’s experience of the medication and whether the wound shows a positive response to the chosen medication.
The patient will need regular medical review and regular blood tests to ensure the medication is not causing additional problems.
Management of pain
Management of pain is essential – this condition can be extremely painful and the patient will need strong analgesia initially often suggested by the Dermatologist. It is important to have treatment for neuropathic pain and anti-neuropathic medication will be required if compression is to be tolerated. Pain will reduce if the inflammatory condition is under control with the medication.
Compression therapy (may include bandages or wraps)
Compression is an essential part of the treatment if you have PG on your legs or feet and this important fact is often missed. Medical management may not be enough on its own to control this condition or any associated swelling. Even if the leg is not very swollen the compression bandage or sock will reduce the level of exudate and make the wounds less wet. You may want to start with mild compression, but increase the level of compression as soon as you can so the limb can benefit from the anti-inflammatory properties of the compression therapy.
The Outlook for Pyoderma Gangrenosum
Pyoderma Gangrenosum can be difficult to treat and this is similar to all inflammatory conditions. Sometimes it can take a while to establish which medication is more effective.
Once the inflammation is under control, the pain will reduce and healing will be seen. If there is significant lower leg swelling, the use of compression therapy is critical and sometimes consistent healing will not be seen until this is used.
There will be scarring once the lesions or ulcers have healed. Scars need to be moisturised daily with a simple emollient.
Prevention of Pyoderma Gangrenosum
The Dermatologist will be able to advise on the risk of recurrence and this will be related to the cause, whether it was spontaneous and how well the ulceration responded to the medication.
It is recommended to keep wearing compression socks to support the leg and reduce the risk of recurrence, especially if there was significant lower leg swelling.
Where’s the harm?
- Pyoderma Gangrenosum on the legs needs compression therapy alongside the medical management
- The powerful anti-inflammatory effects of compression therapy can get missed whilst the doctors focus on establishing the correct medication
- Whilst PG is not caused by venous hypertension, any wound on the leg heals faster with compression therapy
If you have any concerns about the treatment or care you are receiving, it is important to speak up.
Resources
British Association of Dermatologists (Website)
DermNet NZ (Website)
Pyoderma Gangrenosum downloadable leaflet (PDF)
We’ve created a handy downloadable leaflet of the key information on this page so you can easily print it out for personal reference or to hand to a patient or healthcare professional. Or you can also simply forward it on by email.
Other support
Accelerate Based in East London, Accelerate can accept national referrals from your GP / specialist to our world-class centre where we pioneer and trial experimental new treatments for chronic leg ulcers / wounds, lymphoedema and mobility challenges.
Contact details
020 3819 6022
hello@acceleratecic.com
Find out more on the Accelerate website
The Lindsay Leg Club Foundation Promoting and supporting community based treatment, health promotion, education and ongoing care for people who are experiencing leg-related problems - including leg ulcers and other wound care issues.
Contact details
01473 749565
lynn.bullock@legclubfoundation.com
Find out more on the Lindsay Leg Club Foundation website
NHS Choices the official NHS website, which provides vital information and support about leg and foot signs and other symptoms.
Contact details
Call 111 - for non-emergency medical advice
Find out more on the NHS Choices website
Tell us what you think
If there’s anything you want to ask us or tell us, whether it’s a suggestion about our website, a complaint, or a compliment, drop us a line at
support@legsmatter.org










