Overview – what is a venous leg ulcer?
A leg ulcer (LU) is a wound on the lower leg, between the ankle bone and the knee, that does not show signs of healing within 2 weeks. There are a number of causes of leg ulcers, but the majority are caused by damaged veins in the lower leg. These are called venous leg ulcers.
Symptoms – what are the key symptoms of venous leg ulcers?
Your legs may FEEL some, none or all of the following symptoms:
- Pain in your wound
- Pain in the skin around your wound
- Itchy skin
- Dry, tight, red/darker skin around your ankle
- Swollen, tight skin around your ankle or lower leg
- Hardened flesh underneath your skin just above your ankle
- Achy / heavy legs
- Pain in your leg when you put your foot to floor after it has been elevated
Your legs may SHOW some, none or all of the following signs:
- The skin on your leg may be broken and you may have a wound
- The wound may be leaking fluid
- The skin on your leg may have changed colour from your normal and the rest of your skin.
- You may see lots of tiny veins around your ankle or on your foot (this is called ankle flare)
- You may see small white lines on your skin, with red dots in the middle (this is called atrophie blanche)
- You may see varicose veins or thread veins in your leg
- Your leg/foot may have changed shape, be swollen, indented where your socks stop
What do leg ulcers look like?
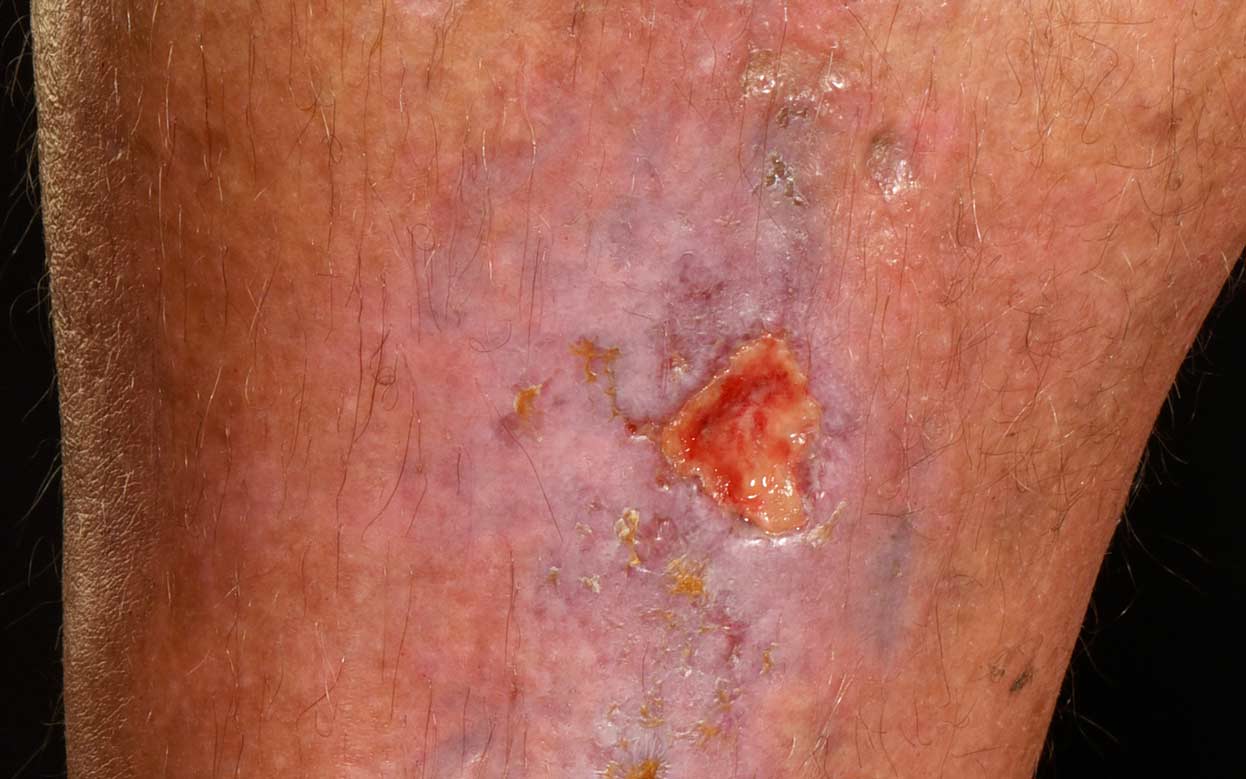
Causes of venous leg ulcers
A venous leg ulcer (VLU) is a break in the skin, between the knee and ankle joint, and is caused by damage to the vein(s) in the lower leg, which become weaker. The weakened vein walls prevent the valves in the veins from closing sufficiently. If the valves cannot close properly, some of the venous blood backflows when the heart beats and the pressure inside the vein increases, pushing small components of the venous blood across the vein wall into the surrounding flesh and skin. This damages the flesh and breaks the skin. Because the vein is weak and leaking, the skin cannot heal.
We have deep veins (inside the leg muscles) and superficial veins (outside the leg muscles) and small veins (perforators) connecting them together. Either or both may be damaged.
Veins can become damaged due to a number of reasons, including;
- An injury
- Previous fracture of the bones in the leg, ankle or foot
- Previous operations
- A clot (DVT)
- Increased abdominal weight (pregnancies or obesity)
- Because the veins get weaker as we get older
Diagnosis – getting diagnosed with a venous leg ulcer and making an appointment
It is important to see your GP / Practice Nurse / District Nurse as soon as possible after your wound appears to get an assessment, diagnosis and have a compression garment prescribed. You should also ask for an appointment if you have had a venous leg ulcer before and you feel one is coming back but the skin hasn’t broken yet.
General Assessment
Your assessment should include questions about:
- Your general health
- Your current and past medical history
- The appearance, shape and feel of your lower leg and your ulcer
Skin Assessment
Your healthcare provider will look for:
- Wound shape, size, depth and the type of tissue in the wound bed
- Ulcer location: what part of the leg is the ulcer on
- Oedema or swelling; how far up the leg does it go? Does it go when you elevate your leg?
- Varicose veins
- Discolouration of the skin on your leg
- Inflammation and wound or skin infection
- Eczema / contact dermatitis
- Changes to the shape of your leg
- Temperature of the skin on your leg, foot and toes
Tests
Your healthcare provider should;
- Listen to the pulses in your foot using a hand held ultrasound scanner
- Test the blood pressure in your arms and legs and compare them together. This is a test of the strength of the arteries in your lower leg and foot. This is often called a ‘Doppler’ Test
- Some people may need to have additional tests depending on the results
- Sometimes you may need a blood test
Treatment – how to treat venous leg ulcers
It is important to see your GP / Practice Nurse / District Nurse as soon as possible to get an assessment, diagnosis and have a compression garment prescribed.
Things to say when booking your appointment:
- If your wound is hot or red, this may be urgent and require care immediately
- How the wounding happened or whether it just spontaneously started
- Make it clear if you have diabetes
- Make it clear that the wound has not healed within two weeks and it’s worrying you
- Let them know if it smells or if it’s painful and what makes this better or worse
Language used
You may hear different words to describe your wound such as ulcer, leg ulcer, sore, laceration, chronic wound and maybe others. Ask your nurse to explain their choice of word and what this may mean for you.
If you’re struggling to get an appointment with your GP, there might be a Leg Club or specialist leg clinic in your area. You may be able to attend these without having to be referred by your GP.
Compression garments and bandages
These include; stiff or elastic bandages, compression stockings and Velcro leg wraps.
Some garments can be applied by you, your family member or a carer with an application aid (eg stockings / hosiery / socks and wraps) and bandages will need to be applied by someone with specific training.
Which compression garment is right for you will depend on:
- The size and location of your ulcer
- The amount of fluid coming from the wound
- The condition of the skin around your wound
- Your pain level
- Your lifestyle
- Who, if anyone, will help you change your dressings and compression garment
Compression garments are essential for when you sit, stand or walk. Strong evidence shows that compression garments and / or venous surgery are the only way to heal VLU’s and to keep them healed. More evidence suggests it is better if you wear them overnight as well.
Surgery
Surgery to remove the damaged vein can improve healing and also reduce the risk of venous ulcers coming back. Surgery can include removing the varicosed vein, or applying heat, ultrasound or foam to seal the damaged vein. Your Vascular Surgeon will discuss with you which is the best option for you once you have had your veins scanned to see which one is damaged.
Dressings
In addition to the compression, your nurse should also advise you on wound care and dressings to keep your wound healthy.
There are many different dressings available and the choice depends on the condition of your wound, which will change as you heal. You may need a few different dressings over the course of your treatment.
Important points
- You should be involved in the decision and your views, choices and how you like to live your life should be listened to
- Leg elevation (ankle above hip level) is important to reduce the pressure inside the veins and will help stop the vein leaking but as soon as you lower your leg or walk the vein will start leaking again unless you are wearing a compression garment
- Ankle exercises and walking normally is also important. This is because when the foot and ankle bend, this helps squeeze the muscles around the veins and this reduces the effects of the high pressure in them
Prevention – how to prevent venous leg ulcers occurring or reoccuring
Venous ulcers can recur if the damaged vein is not supported or removed. Therefore, compression garments should be worn even when the ulcer has healed to stop it coming back.
Leg elevation (ankle above hip level) is important to reduce the pressure inside the veins and will help stop the vein leaking but as soon as you lower your leg or walk the vein will start leaking again unless you are wearing a compression garment.
It is also important to know that when the foot and ankle move, this helps squeeze the muscles around the veins and this reduces the effects of the high pressure in them.
Compression garments are essential for when you sit, stand or walk. Strong evidence shows that compression garments and / or venous surgery are the only way to heal VLU’s and to keep them healed.
Outlook – healing venous leg ulcers
Venous leg ulcers can heal well with the right compression garments. Compression supports the veins and stop them leaking and allow the body to heal the wound. Continuing to wear them when your venous leg ulcer has healed can help reduce the risk of the wound coming back.
Surgery to remove the damaged vein can improve healing and also reduce the risk of venous ulcers coming back.
It is important to wear compression as quickly as possible and to keep wearing it after your venous ulcer has healed.
How can I help my venous leg ulcer heal?
- Make an appointment to see your GP / Practice Nurse or District Nurse as soon as possible to be assessed, get a diagnosis and access treatment that will heal your ulcer
- Wear the compression garments given to you by your health provider
- Elevate your leg with your ankle above your hip level whenever possible – use pillows under the foot of your mattress, while you are lying on a sofa or sitting in a chair with your leg(s) elevated
- Ask to see a Vascular Consultant to have your veins scanned and assessed to see which vein is damaged and if you may benefit from having the damaged one removed. Do this even if you do not end up choosing to have surgery as the scans can find which vein is causing the problem and guide the way forward for your treatment in the future
Harm – the risk factors
Inaction or insufficient action on venous leg ulcers can cause harm. This includes:
- Not checking legs properly or doing basic checks, such as a Doppler test
- Not performing a vascular assessment to determine if suitable for compression
- Not using adequate compression if indicated, can lead to worsening disease
- Not being referred to vascular services for venous intervention if required
If you have any concerns about the treatment or care you are receiving, it is important to speak up.
Resources – for venous leg ulcers
- Lower leg ulcer diagnosis & principles of treatment (PDF), Wounds Australia & European Wound Management Association (EWMA)
- NICE Venous leg ulcers (Website)
- Vascular Society (Website)
- Holistic management of venous leg ulceration (second edition) – Wounds UK (PDF)
- National Wound Care Strategy (NWCSP) Leg Ulcer Recommendations Summary (PDF)
Venous leg ulcer downloadable leaflet (PDF)
We’ve created a handy downloadable leaflet of the key information on this page so you can easily print it out for personal reference or to hand to a patient or healthcare professional. Or you can also simply forward it on by email.
Other support
Some organisations you can contact for further information.
Accelerate Based in East London, Accelerate can accept national referrals from your GP / specialist to our world-class centre where we pioneer and trial experimental new treatments for chronic leg ulcers / wounds, lymphoedema and mobility challenges.
Contact details
020 3819 6022
hello@acceleratecic.com
Find out more on the Accelerate website
British Heart Foundation The British Heart Foundation were founded in 1961 by a group of medical professionals wanting to fund extra research into the causes, diagnosis, treatment and prevention of heart and circulatory disease. Today they are the nation's heart charity and the largest independent funder of cardiovascular research.
Contact details
0300 330 3322
supporterservices@bhf.org.uk
Find out more on the British Heart Foundation website
Diabetes UK Diabetes UK are the leading UK charity for people affected by diabetes it’s their responsibility to lead the fight against the growing crisis. And this fight is one that involves all everyone – sharing knowledge and taking diabetes on together.
Contact details
0345 123 2399
helpline@diabetes.org.uk
Find out more on the Diabetes UK website
The Lindsay Leg Club Foundation Promoting and supporting community based treatment, health promotion, education and ongoing care for people who are experiencing leg-related problems - including leg ulcers and other wound care issues.
Contact details
01473 749565
lynn.bullock@legclubfoundation.com
Find out more on the Lindsay Leg Club Foundation website
Tell us what you think
If there’s anything you want to ask us or tell us, whether it’s a suggestion about our website, a complaint, or a compliment, drop us a line at
support@legsmatter.org











