Overview – varicose veins are swollen and enlarged veins that usually occur on the legs and feet
Lots of people have swollen or ‘varicose’ veins. Varicose veins can make our legs painful, heavy, itchy and swollen. This is because of how blood is pumped around our legs.
Symptoms – what are the key symptoms of varicose veins
What do varicose veins look like?
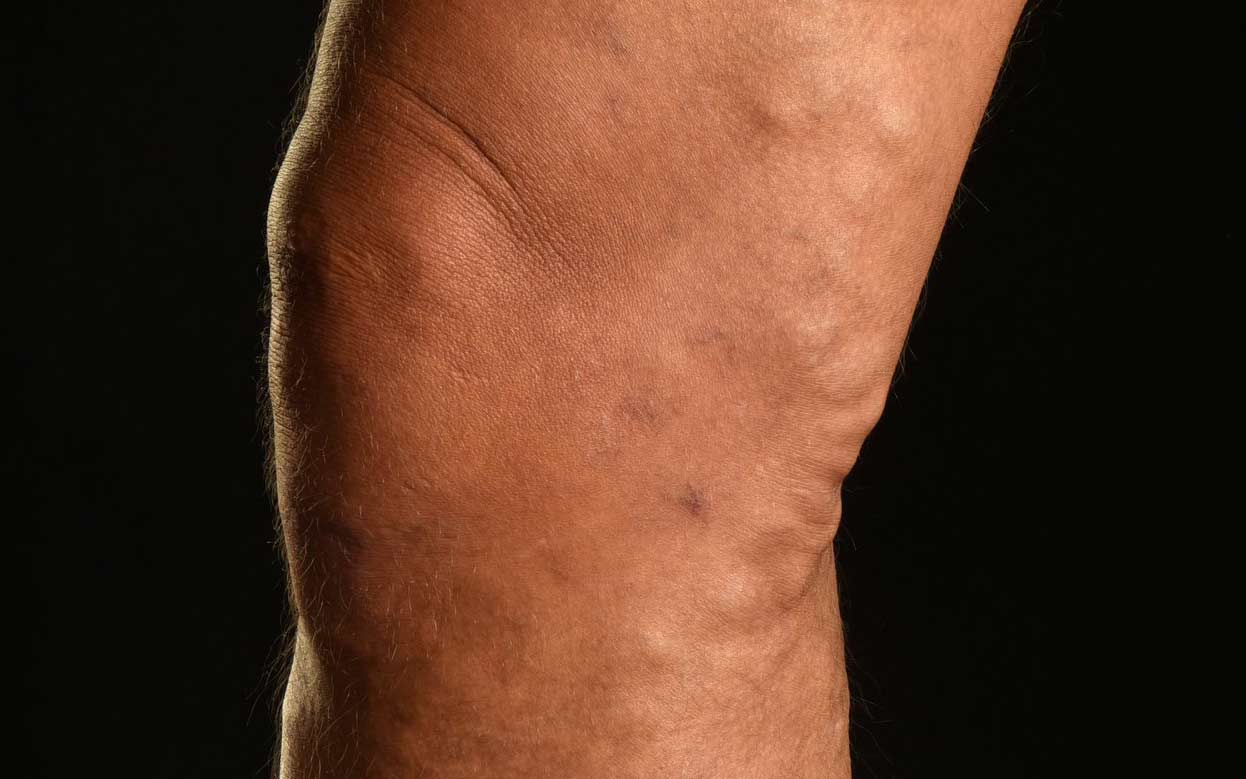 Varicose veins can appear dark blue and stick out from the skin, a little like raised tunnels. They can develop anywhere in the body, but are often found around the legs and ankles.
Varicose veins can appear dark blue and stick out from the skin, a little like raised tunnels. They can develop anywhere in the body, but are often found around the legs and ankles.
Causes – what causes varicose veins?
Peripheral arterial disease
One cause of poor healing in the lower leg is when not enough blood is getting to our feet. Blood travels from our heart to our feet through our arteries. If our arteries become too narrow, our skin will not get enough blood to allow the wound to heal as normal.
Blood is pumped from our heart to the rest of our body through arteries and returns to the heart through our veins. Blood from our lower legs and feet is propelled back to the heart by the heart pumping and by being pushed by the leg and foot muscles as we walk and when our ankle is moved.
Our veins contain one-way valves to prevent backflow or the blood falling back towards our toes. These valves can become weak or damaged leading to venous back flow. When this happens, our veins become so swollen (varicose veins) that blood is forced into the tissue of our skin. The pressure in our veins becomes higher than the pressure in our arteries and the blood flows backwards and collects in the vein. This makes the vein swollen and enlarged. We might also notice that our ankles are swollen, and brown staining appears on our legs.
Many people with varicose veins in the legs have no symptoms but some people find their lower legs are painful or aching, feel swollen and heavy or itchy. Symptoms can often get worse during the day or towards the evening especially around the ankle area. When legs are elevated (such as at nighttime) the swelling often reduces, and symptoms improve.
Diagnosis – getting your varicose veins diagnosed
If your varicose veins are causing pain, heaviness or itching, make an appointment at your GP practice. It might be useful to keep a diary of symptoms that include the things that improve or worsen the symptoms and the time of day that they happen. Remember to remove any nail polish from your toenails before your appointment.
When you see the nurse or doctor, they should:
- Ask about your symptoms and how long you have had problems
- Examine your lower legs
You might also be offered some tests to check for other health problems that can affect your legs, such as diabetes and anaemia.
If your varicose veins are bleeding your GP practice should refer you to a vascular service immediately. Your GP should also refer you to a vascular service if your varicose veins are hard and painful, or causing skin discoloration or itchiness and eczema. This might be sign of problems with the blood flow in the leg so need to be checked out.
If you are referred to a specialist vascular clinic you will may be offered a duplex ultrasound scan to diagnose your varicose veins. This scan uses high-frequency sound waves to produce a picture of the veins and blood flow in your legs.
What to expect at your appointment
You should have a comprehensive assessment of your varicose veins. As mentioned above, if your veins are bleeding you should be immediately referred to a vascular service
You should also be referred if you have the following symptoms:
- Symptomatic primary or symptomatic recurrent varicose veins
- Lower limb‑ skin changes, such as pigmentation or eczema, thought to be caused by chronic venous insufficiency
- Superficial vein thrombosis (characterised by the appearance of hard, painful veins) and suspected venous incompetence
If you have open and healed venous leg ulceration (a break in the skin below the knee that has not healed within 2 weeks) you may also benefit from being referred to a vascular service for assessment of the extent of the venous disease and possible intervention or surgery.. This vascular service assessment should include a duplex ultrasound to confirm the diagnosis of varicose veins and the extent of truncal reflux, and to plan treatment for people with suspected primary or recurrent varicose veins.
Treatment – what treatment will I be offered for varicose veins?
At the initial consultation, you should have the following information:
- An explanation of what varicose veins are
- Probable causes of varicose veins
- The likelihood of progression and possible complications, including deep vein thrombosis, skin changes, leg ulcers, bleeding and thrombophlebitis.
You should also have had advice on any misconceptions that you may have about the risks of developing complications, and be able to discuss possible treatment options, including symptom relief, an overview of interventional treatments and the role of compression.
There are lots of different options for treating varicose veins. These could include the following:
Intervention for varicose veins
Varicose vein surgery is minimally invasive and works by sealing shut or removing the damaged vein so that blood is redirected to healthy veins instead. This can be done by traditional operation or by newer endovenous techniques.
Types of operations / endovenous techniques include:
Endothermal ablation
This works by inserting a wire into the vein and applying heat to seal it shut.
Ultrasound-guided foam sclerotherapy
A chemical – called a sclerosant – is mixed with air or another gas to produce a foam. The foam is injected into the vein and ultrasound is used to check that the foam is going to the right places. The sclerosant in the foam creates scarring inside the vein, which closes it.
Ligation and stripping
This is a surgical procedure susually done under general anaesthetic in a theatre setting. The varicose vein is tied off and physically removed. This type of procedure is not offered in all vascular centres and only performed in specific cases.
Compression therapy (support bandages or socks) for varicose veins
If you have no problems with the blood supply to your legs, compression therapy can be a good way of reducing your symptoms of varicose veins and swelling.
Compression therapy works by applying pressure to the leg to improve the blood supply. The simplest way of doing this is by wearing compression socks, stockings or tights. Compression therapy isn’t a permanent way of treating your varicose veins but can be helpful if none of the other treatments are suitable for you.
Pregnancy and compression therapy
If you’re pregnant and have varicose veins, your healthcare professional should explain how your pregnancy affects varicose veins. They may give you compression stockings to wear. Other treatment for varicose veins is not recommended during your pregnancy.
Outlook for people experiencing varicose veins
Some patients unfortunately do experience a recurrence of varicose veins after surgery and this is known as neorevascularisation. To minimise the chance of recurrence it is advisable to continue wearing compression hosiery, avoid standing for long periods of time and ensure you are taking regular exercise.
Prevention – lifestyle advice for people experiencing varicose veins
Making healthy changes to your lifestyle can help ease the symptoms of varicose veins:
- Maintain a healthy weight
- Take light to moderate exercise, such as swimming or walking for about 30 minutes, at least three times a week
- Avoid standing for a long time
- Avoid hot baths
Harm – the risk factors?
- Failure to treat varicose veins could result in patient suffering and impact on quality of life leading to depression
- Over reliance on pain medication
- Over reliance on nursing workforce
- Hospital admissions
Resources
Clinical guidelines for varicose veins
These guidelines give you a useful overview and more detailed information on the management of varicose veins:
- The NICE guideline for varicose veins (Web page)
- The NICE Clinical Knowledge Summary for Varicose Veins (Web page)
- The Venous Forum of the Royal Society of Medicine have published guidance on management of varicose veins (PDF download)
Research surrounding varicose veins and leg ulcers
You will find lots of research evidence to support practice, including a number of systematic reviews about the management of varicose veins.
Other support
Some organisations you can contact for further information.
British Heart Foundation The British Heart Foundation were founded in 1961 by a group of medical professionals wanting to fund extra research into the causes, diagnosis, treatment and prevention of heart and circulatory disease. Today they are the nation's heart charity and the largest independent funder of cardiovascular research.
Contact details
0300 330 3322
supporterservices@bhf.org.uk
Find out more on the British Heart Foundation website
The Circulation Foundation The Circulation Foundation is the UK’s only dedicated vascular charity. They fund and promote research into the causes, treatment and prevention of vascular disease.
Contact details
020 7205 7151
info@circulationfoundation.org.uk
Find out more on The Circulation Foundation website
NHS Choices the official NHS website, which provides vital information and support about leg and foot signs and other symptoms.
Contact details
Call 111 - for non-emergency medical advice
Find out more on the NHS Choices website
The Society of Vascular Nurses The Society of Vascular Nurses (SVN). The SVN is a professional, membership organisation for vascular nurses throughout the UK who provide optimal care for vascular diseases. Through their culture of sharing, they offer excellence in clinical practice, education, research and professional networking in order to strive for optimal care for patients with vascular disease.
Contact details
Visit SVN
Tell us what you think
If there’s anything you want to ask us or tell us, whether it’s a suggestion about our website, a complaint, or a compliment, drop us a line at
support@legsmatter.org









